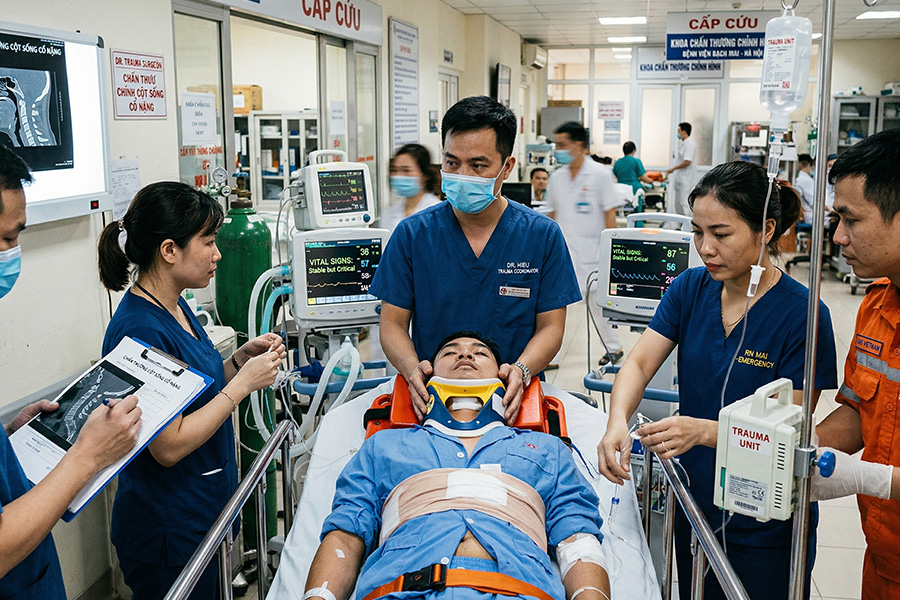
Tourist Spine Injury in Vietnam: Surgery and Repatriation
Severe spinal trauma represents one of the most critical and time-sensitive categories in international medical assistance operations. These cases require immediate diagnostic imaging, rapid surgical decision-making, and seamless coordination between hospitals and assistance providers. This case involves a 1990-born male tourist Kazakhstan who sustained a severe cervical spine injury during a holiday in Vietnam following a fall from a swing. The case demonstrates the complexity of inter-hospital transfer, advanced spinal surgery, postoperative complication management, and international medical repatriation.
Clinical Presentation and Diagnosis
The patient was initially admitted to Vinmec Phu Quoc International Hospital on 24 January 2026.
Upon admission, the clinical findings included:
- Complete paralysis of the lower extremities
- Loss of sensation below the umbilical level
- Severe neurological deficit consistent with spinal cord involvement
Radiological evaluation confirmed an unstable fracture at the C7 level with spinal cord compression.
Given the severity of the condition, conservative management was ruled out, and urgent surgical stabilization was indicated. The patient was transferred to City International Hospital (CIH) in Ho Chi Minh City for advanced neurosurgical care.
Surgical Intervention
On 28 January 2026, a complex anterior cervical procedure lasting approximately seven hours was performed, including:
- C7 corpectomy
- Spinal cord decompression
- Placement of a 25 mm titanium cage
- C6–T1 anterior plating and stabilization
The surgery was completed without intraoperative complications. Hemostasis was achieved, and no surgical drain was required. The wound was closed in layers, ensuring optimal postoperative recovery conditions.
Postoperative Course and Complications
In the early postoperative period, the patient developed pneumonia, requiring intensive care unit (ICU) admission.
Through multidisciplinary management, including respiratory support, antibiotic therapy, and close monitoring, the infection was successfully controlled. The patient was later transferred back to the general ward in stable condition.
This phase highlighted the importance of proactive complication management in high-risk spinal trauma cases.
Medical Repatriation
On 2 February 2026, the patient was clinically assessed and deemed fit for air travel.
Key discharge conditions included:
- Stable neurological status
- Controlled infection
- Overall clinical improvement
Two days later, a planned medical repatriation was conducted. The patient was safely transported to Kazakhstan under medical escort in a business class cabin configuration, ensuring optimal positioning and continuous monitoring.
Outcome and Clinical Significance
The total hospital stay lasted 12 days. This case highlights several critical principles in severe cervical spine trauma management:
- Importance of early surgical decompression
- Necessity of rapid transfer to specialized centers
- Effective management of postoperative complications, particularly pneumonia
- Critical role of ICU-level multidisciplinary care
- Structured and safe international medical repatriation planning
In unstable C7 fractures with spinal cord compression, timely surgical intervention combined with coordinated international assistance can significantly improve neurological and functional outcomes.
This case demonstrates how rapid decision-making, cross-border coordination, and structured clinical pathways directly influence patient prognosis.
Throughout the process, seamless coordination between facilities ensured uninterrupted care from initial admission in Phu Quoc to surgical treatment in Ho Chi Minh City and final repatriation.
Remed Assistance played a key role in ensuring efficient communication between stakeholders, timely clinical escalation, and safe repatriation of the patient in stable condition to his home country.